香港泌尿科專科醫生 — 崔家倫醫生 Dr Chui Ka Lun
Not all patients are the same, Dr Chui will discuss with you and tailor an option of treatment only for you
醫生簡介
提供完整的泌尿外科手術同意書附表,包含詳細的手術說明、風險評估和注意事項。 所有文件均可即時下載,方便醫療人員和患者查閱。
手術同意書附表合集 由崔家倫醫生編輯
手術同意書與風險簡述
1.經尿道激光前列腺剜除術 (HoLEP)
2.經會陰前列腺穿刺活檢 (Transperineal prostate biopsy)
3.精囊內窺鏡手術 (Transurethral seminal vesiculoscopy)
4.輸尿管內窺鏡激光碎石術及雙J管支架置入(Ureterorenoscopic laser lithotripsy + Double J stent insertion)
5.腹腔鏡腎臟全切除術 (Laparoscopic radical nephrectomy)
6.腹腔鏡腎臟部分切除術 (Laparoscopic partial nephrectomy)
7.經尿道膀胱內窺鏡水刀腫瘤整塊切除術 (Bladder tumor Endoscopic Submucosal Dissection)
8.經尿道膀胱腫瘤切除術 (TURBT)
9.軟式輸尿管腎臟鏡激光碎石術及雙J管支架置入 (Flexible URSL + Double J Stent)
10.經皮腎造瘻取石術 (PCNL)
11.體外衝擊波碎石術 (ESWL)
12.雙極經尿道前列腺剜除術 (BipoLEP)
13.軟式膀胱鏡檢查及可能之膀胱活檢 (Flexible cystoscopy + bladder biopsy)
14.經會陰直腸間質保護凝膠注射及前列腺金屬標記植入術 (Transperineal rectal spacer injection + fiducial marker insertion)
15.經會陰直腸間質保護凝膠注射 (Transperineal rectal spacer insertion)
16.經會陰 Barrigel 注射及前列腺金屬標記植入術 (Transperineal Barrigel insertion)
17.一次性包皮切割吻合器環切術 (Disposable Circumcision Anastomat)
18.開放式疝氣補片修補手術 (Open mesh hernia repair)
19.經腹股溝睪丸切除術 (Inguinal orchidecromy)
20.膀胱鏡激光膀胱碎石術 (Cystoscopic bladder stone laser lithotripsy)
21.經尿道前列腺 Memokath 支架置入術 (Prostate Memokath insertion)
22. 睪丸假體植入術
(Testicular Prosthesis Implantation)
23.顯微附睾精子抽吸術 (MESA)
24.顯微睪丸取精術 (Micro-TESE)
25.陰囊水囊腫切除術 (Hydrocelectomy)
26.陰莖繫帶切除/成形術 (Frenulectomy)
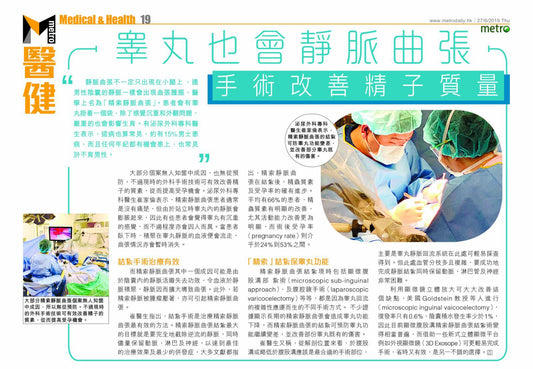
27.經陰囊顯微精索靜脈曲張切除術 (Subinguinal microscopic varicocelectomy)
28.陰莖體外低能量衝擊波治療 (ESWT)
29.陰莖玻尿酸注射增粗術 (Hyaluronic acid penile augmentation)
30.佩羅尼氏症摺疊矯正手術 (Plication surgery for Peyronie's disease)
31.膀胱瓣輸尿管重建手術 (Boari Flap ureteric reimplanation)
32.腹腔鏡輸尿管切開取石術 (Laparoscopic ureterolithotomy)
33.膀胱膨出修補術 (Cystocele repair/ Anterior colporrhaphy)
34.尿道肉阜切除術 (Caruncle excision)
35.卡介苗膀胱內灌注治療 (Intravesical BCG instillation)
36.輸尿管 Memokath 金屬支架置入術 (Ureteric Memokath insertion)
37.腹腔鏡腎上腺切除術 (Laparoscopic adrenalectomy)
38.腹腔鏡臍尿管遺跡切除術 (Laparoscopic urachal remnant excision)
39.陰莖假體植入術
(Penile Prosthesis Implantation)
40. 機器人輔助根治性前列腺切除術 (Robotic-Assisted Radical Prostatectomy)
41. 機器人輔助根治性膀胱切除術合併迴腸導管造口術及骨盆淋巴結清掃術
(Robotic-Assisted Radical Cystectomy with Ileal Conduit and Pelvic Lymph Node Dissection)
42. 前列腺水蒸氣治療術 (Prostate Water Vapor Thermal Therapy)
43. 前列腺提拉術 (Prostatic Urethral Lifting therapy)
44. 腹腔鏡腎輸尿管全切除術 (Laparoscopic Nephroureterectomy)
45. 軟式輸尿管腎臟鏡激光消融腎盂移行細胞癌術 (Flexible Ureteroscopic Laser
Ablation of Renal Transitional Cell Carcinoma)
46. 開放式腰大肌懸吊術合併膀胱瓣輸尿管重建術 (Open Psoas Hitch with Boari
Flap for Distal Ureteric Stricture)
Achievement
A discovery, innovation, or scientific study within the field of surgery
Dr. Chui Ka Lun has been the principal pioneer in introducing and standardizing the transperineal (TP) ultrasound-guided prostate biopsy in Hong Kong, effectively replacing the traditional transrectal (TR) approach. Historically, the transrectal approach was the gold standard but carried a significant risk of severe complications, notably post-biopsy urosepsis, due to the needle passing through the rectum's faecal flora. Dr. Chui initiated the TP approach under local anaesthesia at his institution in 2018. He subsequently co-authored the first comparative study in Hong Kong demonstrating the clinical superiority of the TP approach. His work established a comprehensive, scalable biopsy protocol (ranging from 10 to 24 cores based on prostate size) that could be performed as a day-case procedure under local anaesthesia, completely avoiding rectal mucosa penetration [1] [2].
Has changed clinical practice
Dr. Chui’s foundational work and subsequent publications catalysed a complete paradigm shift in urological practice across Hong Kong. Following his 2018 initiative and the publication of his comparative study in 2019, there was a territory-wide "Trexit" (transrectal exit) movement. By 2019, the transperineal approach had gradually replaced the transrectal route as the standard of care for prostate biopsies in Hong Kong [3]. This shift fundamentally altered how urologists in the region diagnose prostate cancer. Furthermore, the mastery of the transperineal approach laid the essential anatomical and technical groundwork for a wave of downstream surgical innovations. Urologists, now proficient in transperineal access, have successfully introduced multimodality focal therapies, including High-Intensity Focused Ultrasound (HIFU), cryotherapy, Targeted Microwave Ablation (TMA), and NanoKnife (Irreversible Electroporation) [4] [5]. Dr. Chui has also extended this technique to assist in radiation oncology, pioneering the transperineal injection of rectal spacers (SpaceOAR) and fiducial gold markers to protect the rectum during Stereotactic Body Radiation Therapy (SBRT) and proton therapy for pelvic malignancies [6].
Has had a profound impact on patient care
The transition to transperineal prostate biopsy has yielded immediate and profound benefits for patient safety and healthcare economics. The most critical impact is the near-elimination of post-biopsy urosepsis. Previous territory-wide data indicated that TR biopsies resulted in a 5.7% emergency attendance rate and a 3.8% hospitalisation rate, with up to 0.9% of patients requiring ICU admission for severe urosepsis [7]. Dr. Chui's comparative study demonstrated a reduction of infection and fever rates from 4% (requiring 1-week IV antibiotics) down to 0% [1]. This has spared countless patients from life-threatening infections, eliminated the associated psychological trauma, and significantly reduced the financial burden on the public healthcare system by decreasing emergency room visits, hospital bed occupancy, and intensive care admissions. Additionally, the shift has mitigated the growing public health crisis of antimicrobial resistance, as the TP approach dramatically reduces the reliance on broad-spectrum prophylactic antibiotics, such as fluoroquinolones, which were previously mandated for TR biopsies [3].Beyond diagnostics, the downstream innovations facilitated by Dr. Chui’s transperineal techniques have further enhanced patient quality of life. The introduction of transperineal focal therapies allows for the precise eradication of cancer cells while preserving urinary continence and sexual function [4]. The use of transperineal rectal spacers in SBRT and proton therapy has minimized gastrointestinal toxicities, ensuring exceptional tolerability for patients undergoing radiation for localized prostate cancer [6].
Publications
1.Lo KL, Chui KL, Leung CH, Ma SF, Lim K, Ng T, Wong J, Li JKM, Mak SK, Ng CF. "Outcomes of transperineal and transrectal ultrasound-guided prostate biopsy." Hong Kong Medical Journal, 2019 Jun;25(3):209-15. (First published comparative study in HK demonstrating the safety and efficacy of the TP approach).
2.Lo KL, Leung D, Lai Z, Li C, Ma SF, Wong J, Yuen KK, Li J, Chiu P, Mak SK, Wong J, Ng CF. "Picture-in-picture video demonstration of systematic transperineal prostate biopsy." Hong Kong Medical Journal, 2021 Aug;27(4):304-5. (Demonstrates the standardized TP biopsy protocol initiated by Dr. Chui).
3.Chiu PKF, Ng CF. "Primum non nocere (first, to do no harm) in prostate biopsy." Hong Kong Medical Journal, 2019 Oct;25(5):344-5. (Editorial highlighting the paradigm shift to TP biopsy in HK, citing Dr. Chui's work).
4.Yee CH, Chiu PKF, Liu AQ, Wong HF, Chan WHC, et al. "Multimodality focal therapy for prostate cancer: outcome of the à la carte approach in clinical practice." Prostate International, 2025.
5.Chiu PKF, Chan CH, Yee CH, Lau SY, et al. "Transperineal targeted microwave ablation (TMA) of localized prostate cancer guided by MRI-ultrasound fusion and organ-based tracking: a pilot study." Prostate Cancer and Prostatic Diseases, 2023.
6.Poon DMC, et al. "One-year clinical outcomes of MR-guided stereotactic body radiation therapy with rectal spacer for patients with localized prostate cancer." World Journal of Urology, 2024.
7.Cheng KC, Lam WC, Chan HC, et al. "Emergency attendances and hospitalisations for complications after transrectal ultrasound-guided prostate biopsies: a five-year retrospective multicentre study." Hong Kong Medical Journal, 2019 Oct;25(5):349-55.
References:
[1]: https://www.hkmj.org/abstracts/v25n3/209.htm
[2]: https://www.hkmj.org/abstracts/v27n4/304.htm
[3]: https://www.hkmj.org/abstracts/v25n5/344.htm
[4]: https://www.sciencedirect.com/science/article/pii/S2287888225000406
[5]: https://www.nature.com/articles/s41391-022-00577-8
[6]: https://link.springer.com/article/10.1007/s00345-024-04784-x
貢獻
外科領域的發現、創新或科學研究
崔家倫醫生是香港引入並標準化經會陰前列腺穿刺活檢(Transperineal ultrasound-guided prostate biopsy)的主要先驅,成功取代了傳統的經直腸(Transrectal)穿刺方法。歷史上,經直腸穿刺一直被視為黃金標準,但由於穿刺針需要穿過含有糞便細菌的直腸,因此帶有嚴重的併發症風險,特別是活檢後的尿道敗血症(urosepsis)。崔醫生於2018年在其所屬醫院率先開展了在局部麻醉下進行的經會陰穿刺活檢。隨後,他共同發表了香港首份比較研究,證明了經會陰方法的臨床優越性。他的工作建立了一套全面且可擴展的活檢方案(根據前列腺大小進行10至24針穿刺),該方案可以在局部麻醉下作為日間手術進行,完全避免了穿透直腸黏膜 [1] [2]。此外,作為國安導師,崔醫生積極推動香港醫療融入大灣區,並在泌尿科界別引入了包括經會陰前列腺穿刺活檢在內的多項創新技術。
改變了臨床實踐
崔醫生的基礎工作及其隨後的發表文獻,促成了香港泌尿科實踐的全面典範轉移。繼他2018年的倡議及2019年比較研究的發表後,香港出現了全港性的「Trexit」(退出經直腸穿刺)運動。到了2019年,經會陰方法已逐漸取代經直腸途徑,成為香港前列腺活檢的標準護理 [3]。這一轉變從根本上改變了該地區泌尿科醫生診斷前列腺癌的方式。此外,對經會陰方法的掌握,為後續一系列的外科創新奠定了重要的解剖學和技術基礎。現時精通經會陰途徑的泌尿科醫生,已成功引入了多模式局部治療(multimodality focal therapies),包括高強度聚焦超聲波(HIFU)、冷凍治療(Cryotherapy)、靶向微波消融(Targeted Microwave Ablation, TMA)以及納米刀(NanoKnife / 不可逆電穿孔) [4] [5]。崔醫生亦將這項技術擴展至輔助放射腫瘤科,率先透過經會陰注射直腸隔離凝膠(SpaceOAR)和植入黃金標記(fiducial gold markers),在盆腔腫瘤的立體定位放射治療(SBRT)和質子治療期間保護直腸 [6]。
對病人護理產生深遠影響
過渡至經會陰前列腺穿刺活檢,為病人安全和醫療經濟帶來了即時且深遠的益處。最關鍵的影響是幾乎消除了活檢後的尿道敗血症。過往的全港數據顯示,經直腸活檢導致5.7%的急症室求診率和3.8%的住院率,高達0.9%的病人因嚴重的尿道敗血症需要入住深切治療部(ICU) [7]。崔醫生的比較研究表明,感染和發燒率從4%(需要一週的靜脈注射抗生素)降至0% [1]。這使得無數病人免受危及生命的感染,消除了相關的心理創傷,並透過減少急症室求診、醫院病床佔用和深切治療部入院率,大幅減輕了公營醫療系統的財政負擔。此外,由於經會陰方法大幅減少了對廣效預防性抗生素(如氟喹諾酮類,以往經直腸活檢必須使用)的依賴,這一轉變亦緩解了日益嚴重的抗菌素耐藥性公共衛生危機 [3]。除了診斷方面,由崔醫生的經會陰技術所促進的下游創新,進一步提升了病人的生活質素。經會陰局部治療的引入,使得在精確根除癌細胞的同時,能夠保留病人的尿失禁控制和性功能 [4]。在SBRT和質子治療中使用經會陰直腸隔離凝膠,已將胃腸道毒性降至最低,確保接受局部前列腺癌放射治療的病人具有極佳的耐受性 [6]。
其他崔家倫醫生的網站連結
泌尿科學術臨床研究
urojournal.org
泌尿科疾病公眾教育
urologyhk.org
香港首本泌尿科繪本
uroadventure.org